This elastic property is the largest contributing factor to the viscoelastic behavior of blood. The red blood cells occupy about half of the volume of blood and possess elastic properties. 
Viscoelastic fluids make up a larger class of fluids called non-Newtonian fluids. As the heart contracts, mechanical energy is transferred from the heart to the blood a small part of the energy is dissipated by the viscosity of the suspension, another part is stored as elastic energy in the red blood cells, and the remaining energy is used to drive blood circulation and is thus converted to kinetic energy. 
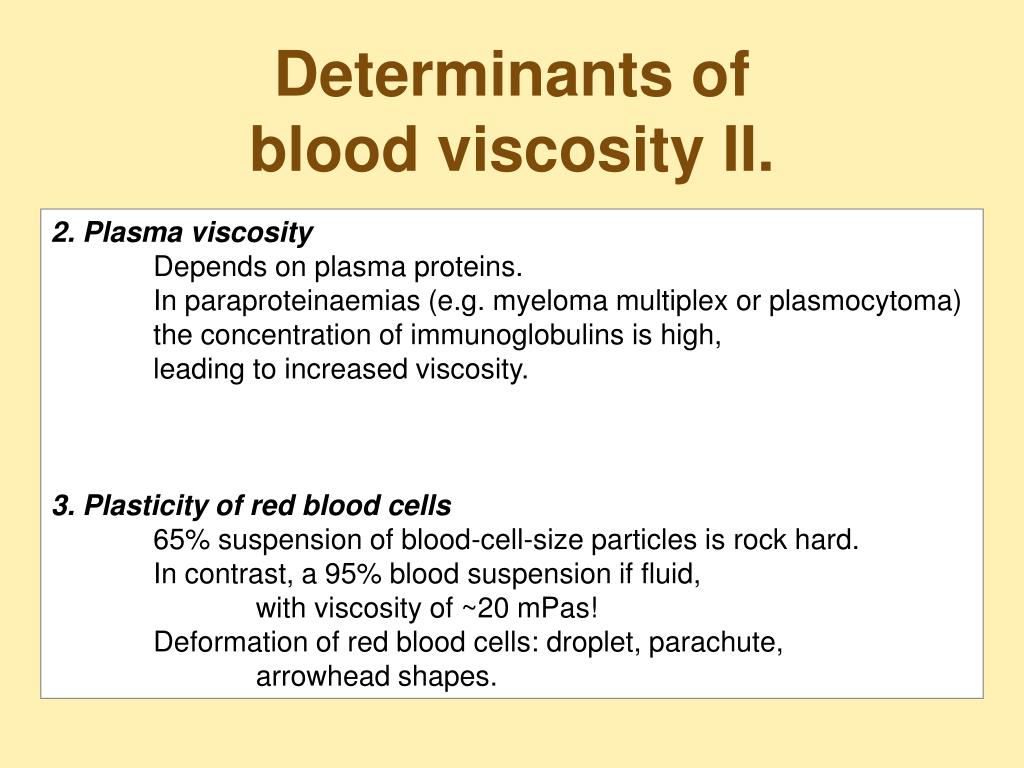
The viscous component arises primarily through the viscosity of blood plasma, while the elastic component arises from deformation of the red blood cells. Blood viscoelasticity īlood is a viscoelastic fluid, meaning that it possesses both viscous and fluid characteristics. Μ = ( 3 ∼ 4 ) ⋅ 10 − 3 P a ⋅ s īlood viscosity can be measured by viscometers capable of measurements at various shear rates, such as a rotational viscometer. s), the viscosity of blood at 37 ☌ is normally 3 × 10 −3 to 4 × 10 −3, respectively 3 - 4 centi poise (cP) in the centimetre gram second system of units.įurthermore, elevation of plasma viscosity correlates to the progression of coronary and peripheral artery diseases. Many conventional cardiovascular risk factors have been independently linked to whole blood viscosity.Ĭardiovascular risk factors linked independently to whole blood viscosity Īnemia can reduce blood viscosity, which may lead to heart failure. This is particularly important in hypothermia, where an increase in blood viscosity will cause problems with blood circulation. Other factors influencing blood viscosity include temperature, where an increase in temperature results in a decrease in viscosity. This will lead to decreased oxygen delivery. When the hematocrit rises to 60 or 70%, which it often does in polycythemia, the blood viscosity can become as great as 10 times that of water, and its flow through blood vessels is greatly retarded because of increased resistance to flow. This relationship becomes increasingly sensitive as hematocrit increases. One unit increase in hematocrit can cause up to a 4% increase in blood viscosity. Nevertheless, hematocrit has the strongest impact on whole blood viscosity. Plasma's viscosity is determined by water-content and macromolecular components, so these factors that affect blood viscosity are the plasma protein concentration and types of proteins in the plasma. The primary determinants of blood viscosity are hematocrit, red blood cell deformability, red blood cell aggregation, and plasma viscosity. These functions of the cardiovascular system are directly related to vascular resistance, preload, afterload, and perfusion, respectively. This biophysical property makes it a critical determinant of friction against the vessel walls, the rate of venous return, the work required for the heart to pump blood, and how much oxygen is transported to tissues and organs. It can also be described as the thickness and stickiness of blood. Blood viscosity also increases with increases in red cell aggregability.īlood viscosity is a measure of the resistance of blood to flow. Contrarily, blood viscosity increases when shear rate goes down with increased vessel diameters or with low flow, such as downstream from an obstruction or in diastole. Therefore, blood is a shear-thinning fluid. Blood becomes less viscous at high shear rates like those experienced with increased flow such as during exercise or in peak- systole. As such, the viscosity of blood varies with shear rate. Because of that, blood behaves as a non-Newtonian fluid. Red blood cells have unique mechanical behavior, which can be discussed under the terms erythrocyte deformability and erythrocyte aggregation. Blood viscosity is determined by plasma viscosity, hematocrit (volume fraction of red blood cell, which constitute 99.9% of the cellular elements) and mechanical properties of red blood cells. Alterations of these properties play significant roles in disease processes. Proper tissue perfusion can occur only when blood's rheological properties are within certain levels. Hemorheology, also spelled haemorheology (from Greek ‘αἷμα, haima ' blood' and rheology, from Greek ῥέω rhéō, ' flow' and -λoγία, -logia 'study of'), or blood rheology, is the study of flow properties of blood and its elements of plasma and cells. ( December 2020) ( Learn how and when to remove this template message) Please help improve this article if you can. The specific problem is: the article is full of duplicated informations in different sections. This article may require cleanup to meet Wikipedia's quality standards. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
